We present the case of a 48-year-old woman with an ostium secundum atrial septal defect corrected in childhood who was diagnosed with noncompaction cardiomyopathy via echocardiography and who had episodes of nonsustained ventricular tachycardia and complete atrioventricular block.
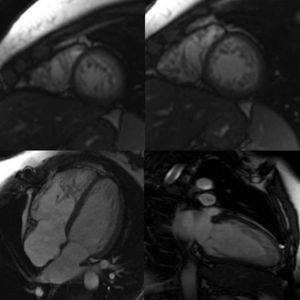
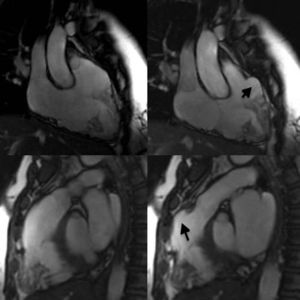
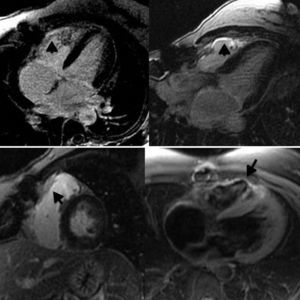
Cardiac magnetic resonance imaging confirmed the diagnosis of noncompaction cardiomyopathy and revealed inferolateral and anteroseptal medioapical hypertrabeculation in the left ventricle with a noncompaction/compaction ratio of 2.97 (11.0 vs 3.7mm) (Figure 1). The left ventricular systolic function was normal. Slight dilatation was also observed of the basal and medial segments of the right ventricle (end-diastolic volume index: 95mL/m2), as well as medioapical hypertrabeculation and microaneurysms in the anterolateral and inferior wall. The right ventricular outflow tract showed an aneurysmatic region of 40mm (Figure 2, arrows; ). The ejection fraction was slightly reduced. Fatty infiltration was also seen in the anterior medioapical wall and the aneurysmatic region, in addition to pathological retention of gadolinium in these areas (Figure 3, arrows), fulfilling the morphological criteria for arrhythmogenic right ventricular dysplasia.
A genetic study identified a novel Glu167Lys mutation in the NKX-2 gene (related to septal defects, bradyarrhythmias, and tetralogy of Fallot) that was also present in her son, who had an ostium secundum atrial septal defect and noncompaction cardiomyopathy, and her daughter, who had pulmonary atresia with ventricular septal defect and had received an implantable cardioverter defibrillator due to ventricular fibrillation. The patient also had a Tyr403Cys mutation in the DSP gene that probably modified the phenotype. Our case illustrates the usefulness of cardiac magnetic resonance imaging to detect ⿿overlapping⿿ morphological findings of distinct cardiomyopathies.