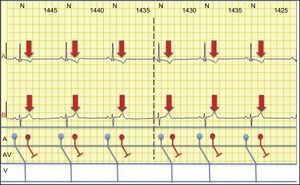
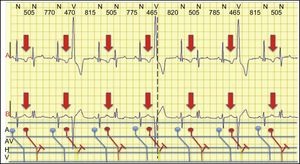
The correct solution is number 4. Figure 1 shows atrial T wave activity, with atrioventricular block, reset of sinus rhythm, and subsequent symptomatic bradycardia. Figure 2 shows the same sequence, with atrioventricular conduction, both of sinus rhythm and extrasystoles, without bradycardia or symptoms. Of note is the perfect alternans of right and left branch aberration. Cohen et al.1,2 described this phenomenon as split atrial activity and explained it by the presence of an occult retrograde penetration of the His-Purkinje system.
In the absence of extrasystoles, the patient showed stable sinus rhythm, with adequate chronotropic control. Therefore, the patient does not have sinus dysfunction or structural branch block alternans. Instead, the abnormality is caused by atrial extrasystoles, leading to retrograde capture of the conduction system. Thus, neither pacemaker placement (answer 1, incorrect) nor drug withdrawal (answer 2, incorrect) would be justified. Likewise, sinoatrial block is not present (answer 3, incorrect) as the electrocardiographic criteria are not met.
.